| ||||
Vitamin D3 deficiency and its role in colds, influenza and COVID 19 infections
Vitamin D3 has a major impact on the outcome of COVID -19 InfectionsinV
Summary of Findings
It has long been known that Vitamin D3 protects against colds and flu since a major global study was published in 2017. (182) "The bottom line is that the protective effects of vitamin D supplementation are strongest in those who have the lowest vitamin D levels.
Overall, the reduction in risk of acute respiratory infection induced by vitamin D was on a par with the protective effect of the injectable 'flu vaccine against 'flu-like illnesses (182)
Recent studies have (183, 184) demonstrated a connection between vitamin D levels and mortality from COVID-19.
May 2020 Patients with severe Vitamin D deficiency are twice a likely to experience severe COVID infection complications including death (191)
In June 2020 three additional studies examining the relationship between the severity of COVID-19 infections and the patients vitamin D levels suggests that adequate vitamin D levels could prevent the disease becoming severe in 90% of cases and reduce patients risk of dying from the infection by 96% (185, 186, 187) See details below.
Feb 21 USA politician calls for CDC and FDA to back Vitamin D for COVID infections (194)
July 2021 Vitamin D determines Severity in COVID-19:
- Researchers Urge Government to Change Advice on Vitamin D and COVID infections (1)
- Over 200 Scientists & Doctors Call for Increased Vitamin D Use To Combat COVID-19 (193)
Review of Findings in Influenza and COVID-19 Infections in relation to Vitamin D Levels
There is important data that suggests maintaining your Vitamin D3 level in the optimal range protects you from colds and flu. Some of this information is not new, but has largely been ignored. The emergence of the COVID-19 pandemic has rekindled interest in these data and led to new data being generated which is very convincing.
Dr. Cannel, founder of the Vitamin D3 Council, was perhaps the first to publish on the possible role of vitamin D in colds and influenza publishing two paper, the first in 2006 in the journal Epidemiology and Infection and the second in 2008 in Virology Journal. Click on these links for summaries of these papers. Dr. Cannel proposed in these publications that many of the characteristics of winter colds and influenza can be correlated with low Vitamin D3 levels.
In February 2009 another paper published in the Archives of Internal Medicine (179) strongly supported these observations. In this study Vitamin D3 levels were measured in over 19,000 Americans, and those with the lowest levels reported having significantly more cases of colds or flu. Dr Adit Ginde, the lead author of the paper, offered the following conclusion:
"The findings of our study support an important role for Vitamin D3 in prevention of common respiratory infections, such as colds and the flu. Individuals with common lung diseases, such as asthma or emphysema, may be particularly susceptible to respiratory infections from Vitamin D3 deficiency."
In addition, two studies also published in 2009 have suggested that low Vitamin D3 levels in newborns make them more susceptible to viral infections. In the first study (180) over 87 percent of all newborns with acute lower respiratory tract infections had vitamin D3 levels lower than 20 ng/ml, which is a severe deficiency state. The second study (181) concluded:
"Based on the available evidence showing a strong connection between Vitamin D3, infections and immune function in children, Vitamin D3 supplementation may be a valuable therapy in pediatric medicine".
Then in 2017 a large meta analysis was published in the BMJ The results are based on a new analysis of raw data from around 11,000 participants in 25 clinical trials conducted in 14 countries including the UK, USA, Japan, India, Afghanistan, Belgium, Italy, Australia and Canada. Individually, these trials yielded conflicting results, with some reporting that vitamin D protected against respiratory infections, and others showing no effect.
Lead researcher Professor Adrian Martineau from QMUL said: "This major collaborative research effort has yielded the first definitive evidence that vitamin D really does protect against respiratory infections. Our analysis of pooled raw data from each of the 10,933 trial participants allowed us to address the thorny question of why vitamin D 'worked' in some trials, but not in others.
"The bottom line is that the protective effects of vitamin D supplementation are strongest in those who have the lowest vitamin D levels, and when supplementation is given daily or weekly rather than in more widely spaced doses.
Daily or weekly supplementation halved the risk of acute respiratory infection in people with the lowest baseline vitamin D levels, below 25 nanomoles per litre (nmol/L). However, people with higher baseline vitamin D levels also benefited, although the effect was more modest (10 per cent risk reduction). Overall, the reduction in risk of acute respiratory infection induced by vitamin D was on a par with the protective effect of injectable 'flu vaccine against 'flu-like illnesses.
Vitamin D and COVID infections
Following the outbreak of COVID-19 pandemic two studies demonstrated an association between vitamin D levels and mortality from COVID-19 infections. The first from Trinity College Dublin (183) shows that, counter intuitively, countries at lower latitude and typically sunny countries, such as Spain and Northern Italy, had low concentrations of vitamin D and high rates of vitamin D deficiency. These countries also experienced the highest infection and death rates in Europe.
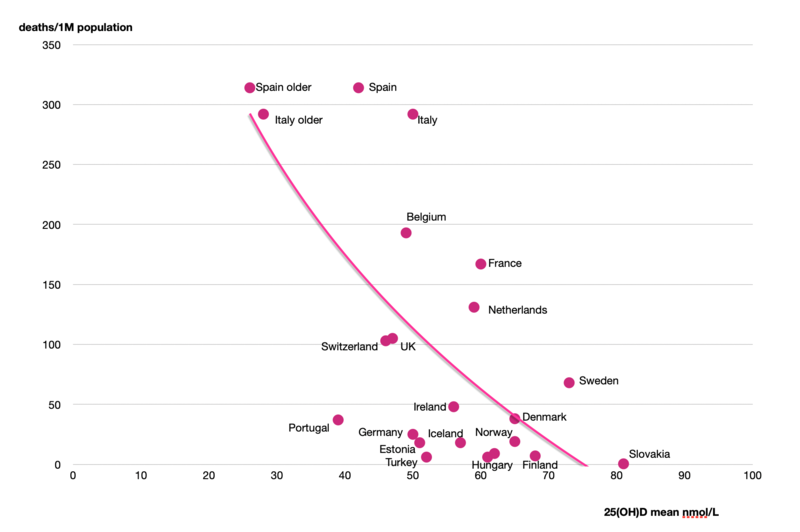
The northern latitude countries of Norway, Finland and Sweden, have higher vitamin D levels despite less UVB sunlight exposure, because supplementation and fortification of foods is very common and has been in place for many years. These Nordic countries have significantly lower COVID-19 infection and death rates. Norway and Finland which had the highest vitamin D levels hardly had any deaths, compared to 300 deaths per million population in Spain which had the lowest vitamin D levels. The correlation between low vitamin D levels and death from COVID-19 is statistically significant. A second study conducted by Northwestern University showed exactly the same result. (184)
In June 2020 three additional studies examining the relationship between the severity of COVID-19 infections and patients vitamin D levels suggests that adequate vitamin D levels could prevent the disease becoming severe in 90% of cases and reduce patients risk of dying from the infection by 96% (185, 186, 187)
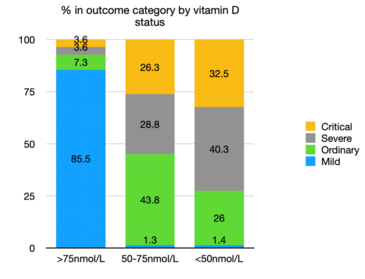
In a study conducted in COVID-19 patients in the Philippines it was found that 72.8% of patients with vitamin D levels of less than 50nmol/L had severe or critical conditions compared to only 7.2% of patients with vitamin D levels of greater than 75nmol/L (185) This was a retrospective multicentre study of 212 cases with laboratory confirmed infection with COVID-19. Of the 212 cases the majority had ordinary clinical outcomes. Vitamin D levels were lowest in the critical cases and highest in the mild cases. The vitamin D status was shown to be significantly associated with the clinical outcome.
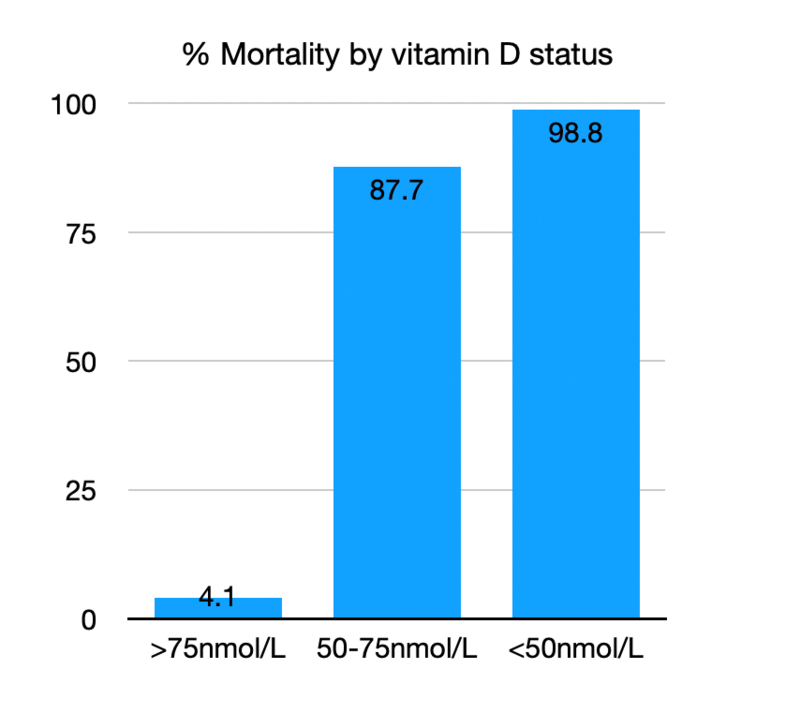
In another study conducted in Indonesia (186) in 780 patients with laboratory confirmed infection with COVID-10 the mortality rate was 98.8% in patients with a vitamin D level below 50nmol/L and only 4.1% in patients with vitamin D levels above 75nmol/L. Results revealed that the majority of the deaths were males and older and had pre-existing conditions and below normal Vitamin D levels. Univariate analysis revealed that older and male cases with pre-existing conditions and below normal vitamin D levels were associated with increasing odds of death. When controlling for age, sex, and comorbidity, Vitamin D status is strongly associated with COVID -19 mortality outcomes.
Finally, the third study (187) looked at the mortality rate by country compared to the average vitamin D level. Clearly those countries with the highest vitamin D levels had the lowest mortality rates for COVID -19 infections.
I
It is therefore recommended that vitamin D supplementation be aimed at increasing serum 25-hydroxyvitamin D [25(OH)D] levels to 40-60 ng/ml (100-150 nmol/l), which would require daily doses up to 4000 to 5000 IU/d vitamin D3.(189)
There is also significant laboratory data to substantiate these findings. In a review article Cell Defenses and the Sunshine Vitamin published in Scientific American in 2007, the authors explain how Vitamin D3 has been shown to activate multiple genes in just about every tissue in the human body. In particular, Vitamin D3 activates two genes that encode antimicrobial peptides called cathelicidin and defensin beta 2. These small proteins act as natural antibiotics against a wide spectrum of bacteria, viruses and fungi. In studies conducted with cultured human cells they found that exposure to Vitamin D3 caused an increase in the cells ability to manufacture both the defensin beta 2 peptide and cathelicidin. In some cell types the rise in cathelicidin production was dramatic.
Clearly, both laboratory and clinical data supports the concept that maintaining a high level of Vitamin D3 may protect from both colds and flu. Now the COVID -19 pandemic has led to studies which even more strongly demonstrate the role of Vitamin D in these infections.
This relationship with Vitamin D should perhaps not come as a surprise. An article by Richard Hobday entitled "Coronavirus and the Sun: a Lesson from the 1918 Influenza Pandemic" detailed how the patients of the 1918 epidemic were treated as were TB patients by being exposed to the sun when ever possible! (190)
The products and the claims made about specific products on this site have not been evaluated by the United States Food and Drug Administration and are not intended to diagnose, treat, cure or prevent disease. The information provided on this site is for informational purposes only and is not intended as a substitute for advice from your physician or other health care professional. You should consult with a healthcare professional before starting any diet, exercise or supplementation program, before taking any medication, or if you have or suspect you might have a health problem
Copyright 2011: Vitamin D3 World | Vitamin D3. All Rights Reserved.